Understanding Your Options When Pain Persists Despite Treatment
If you’ve tried medications, physical therapy, or even surgery but still live with daily pain, you’re not alone. Chronic pain can be frustrating—especially when standard treatments don’t provide enough relief.
In such cases, your doctor may discuss spinal cord stimulation for chronic pain as a potential next step. This therapy focuses on changing how pain is experienced, rather than fixing the underlying cause. For some patients, it may offer meaningful relief and improved quality of life.
Key Takeaways
- Spinal cord stimulation is a minimally invasive therapy used to help manage chronic pain.
- It works by modifying pain signals before they reach the brain.
- A trial of spinal cord stimulation is typically done first to evaluate effectiveness.
- It may benefit patients with nerve-related pain, especially after spine surgery.
- Results vary, and understanding risks and expectations is important before deciding.
What Is Spinal Cord Stimulation?
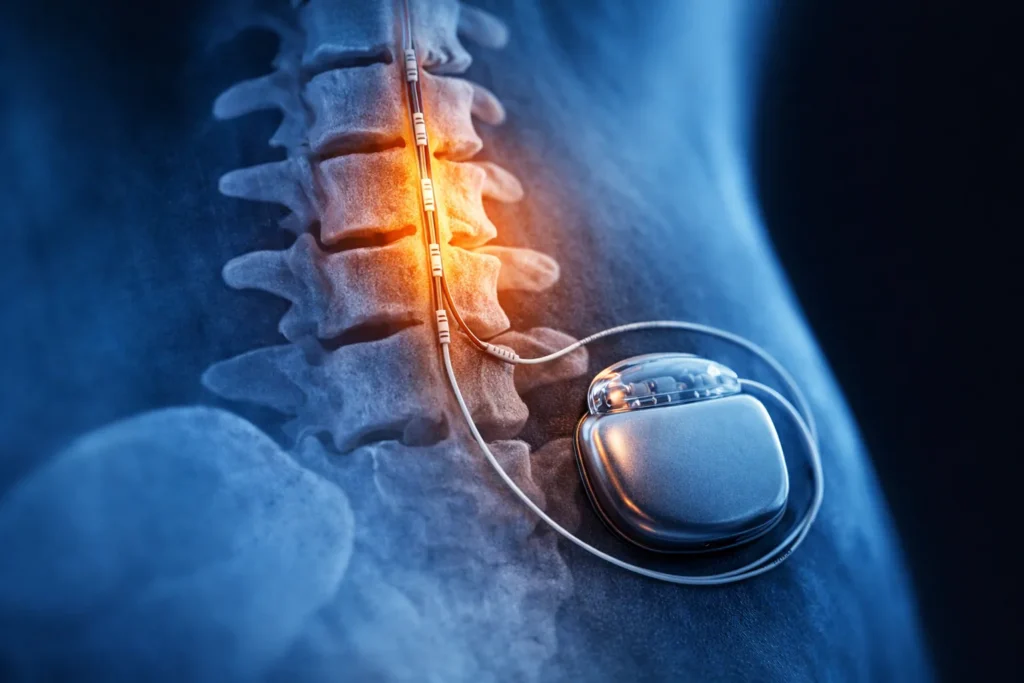
Spinal cord stimulation (SCS) is a treatment that uses a small implanted device called a spinal cord stimulator to help manage chronic pain.
The device sends mild electrical signals to the spinal cord. These signals can interfere with pain messages traveling to the brain, which may reduce how strongly pain is felt.
This approach is commonly considered within broader pain management strategies when other treatments have not provided sufficient relief.
How Does Spinal Cord Stimulation Work?
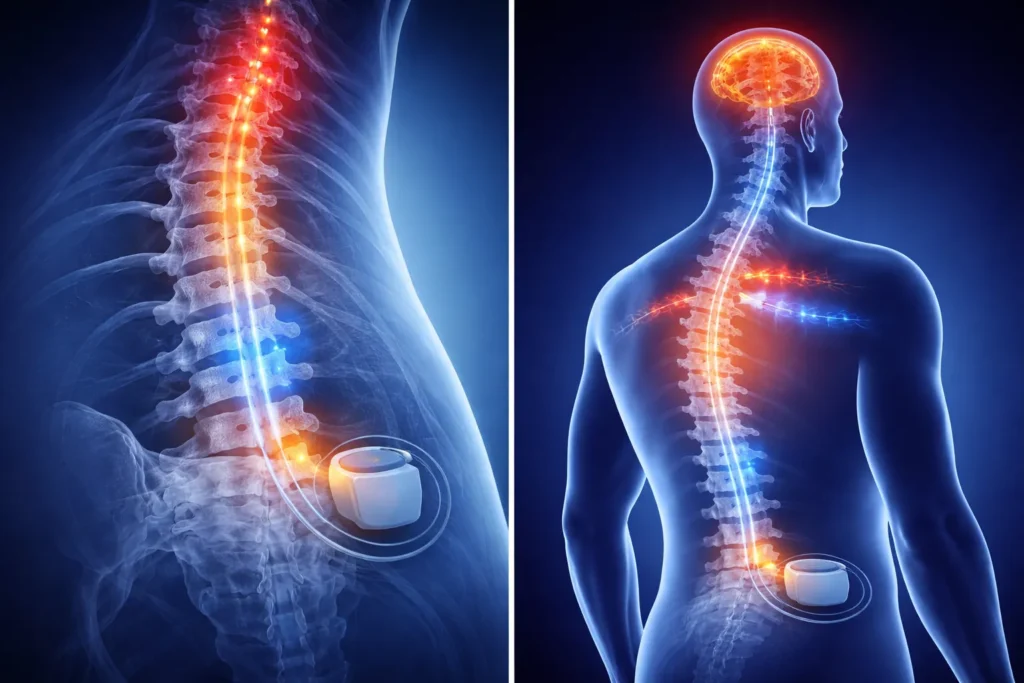
Pain signals travel through the spinal cord to the brain. Spinal cord stimulation therapy works by modifying these signals before they are processed.
Here’s how it works:
- Thin wires (called leads) are placed near the spinal cord
- A small device generates controlled electrical impulses
- These impulses disrupt or alter pain signals
This is particularly helpful for neuropathic pain, which is often described as burning, tingling, or shooting pain.
This matters because nerve-related pain often does not respond well to standard treatments like medications alone.
Who Is a Candidate for Spinal Cord Stimulation?
Your doctor may consider spinal cord stimulation for chronic pain if:
- Pain has lasted longer than 3–6 months
- The pain is nerve-related
- Other treatments (medications, injections, therapy) have not provided enough relief
- Daily activities are significantly affected
It may be used for conditions such as back pain, neuropathic pain, or for failed back surgery syndrome.
When Is Spinal Cord Stimulation Recommended?
It is usually recommended after conservative treatments have failed, and in some cases, as an alternative to repeat surgery.
A full evaluation is typically required to ensure the treatment is appropriate.
Who May Not Be a Suitable Candidate?
Spinal cord stimulation may not be appropriate for everyone. Your doctor may advise against it if you have:
- An active infection
- Untreated psychological conditions that may affect outcomes
- Difficulty managing or operating the device
- Expectations of complete or immediate pain relief
Discussing these factors openly with a qualified provider is important—consider consulting one of the specialists listed on the providers page.
What Is the Spinal Cord Stimulator Procedure Like?
Step 1: Trial Phase
A spinal cord stimulator trial is performed before permanent implantation.
- Temporary leads are placed under the skin
- The device is tested for several days
- You monitor how much pain relief you experience
This step is important because it helps determine whether the therapy is likely to work for you.
Step 2: Permanent Implant
If the trial is successful:
- A small generator is implanted under the skin
- Leads are positioned near the spinal cord
- The system can be adjusted externally
The procedure is typically minimally invasive and performed under medical supervision.
Potential Benefits of a Spinal Cord Stimulator
Many patients experience:
- Reduction in pain intensity
- Improved ability to perform daily activities
- Better sleep
- Reduced reliance on pain medications in some cases
However, results vary, and some patients may experience partial relief rather than complete pain reduction.
Risks, Side Effects, and Limitations
Understanding spinal cord stimulator risks is essential before making a decision.
Possible Risks Include:
- Infection
- Lead movement or device malfunction
- Pain at the implant site
- Need for additional procedures
Spinal Cord Stimulator Side Effects
- Tingling or unusual sensations
- Incomplete pain relief
- Rare complications such as nerve irritation
It’s important to note that this therapy manages symptoms—it does not cure the underlying condition.
Spinal Cord Stimulation vs Other Treatments
Spinal Cord Stimulation vs Surgery
- Surgery aims to correct structural issues
- SCS focuses on modifying pain signals
- SCS may be considered if surgery has not worked or is not preferred
Spinal Cord Stimulation vs Medication
- Medications affect the whole body
- SCS targets pain signals at the spinal level
- Some patients may reduce medication use under medical supervision
Alternatives to Spinal Cord Stimulation
- Physical therapy
- Medications
- Nerve blocks or injections
- Behavioral pain management approaches
Exploring alternatives helps ensure that SCS is considered at the right stage of treatment.
What to Expect After the Procedure
Recovery is usually gradual and varies from person to person.
- Mild soreness at the implant site
- Temporary activity restrictions
- Follow-up visits to adjust the device
Recovery after spinal cord stimulator surgery often allows a return to routine activities within a few weeks, depending on your doctor’s advice.
Is This Right for You?
Deciding whether spinal cord stimulation for chronic pain is appropriate depends on your individual situation.
You may consider discussing this option with your doctor if:
- Your pain has not improved with other treatments
- The pain significantly affects your quality of life
- You are open to trying a reversible, trial-based therapy
You may want to explore other options first if:
- Your pain is not nerve-related
- Conservative treatments have not been fully tried
- You are unsure about having an implanted device
Many patients ask, “Is spinal cord stimulation worth it?”
For some, it may provide meaningful relief and improved function. For others, the benefit may be limited.
A detailed conversation with an Interventional Pain Specialist can help you weigh the potential benefits, risks, and expectations.
Frequently Asked Questions
What is a spinal cord stimulator?
A spinal cord stimulator is a small implanted device that sends electrical impulses to the spinal cord to help manage pain.
How long is the recovery after spinal cord stimulator surgery?
Recovery after spinal cord stimulator surgery usually takes a few weeks. Patients are often advised to avoid heavy lifting, bending, or twisting during early healing to reduce the risk of lead movement.
What is the success rate of a spinal cord stimulator?
The spinal cord stimulator success rate varies, but many studies suggest that a significant number of patients experience meaningful pain reduction (often around 50% or more). The trial phase is a key indicator of whether the therapy is likely to be effective for an individual.
What is the cost of a spinal cord stimulator?
The cost of spinal cord stimulator can vary depending on the device, procedure, and insurance coverage. It’s best to discuss this with your healthcare provider and insurance company.
Can the spinal cord stimulator be adjusted?
Yes, the device can be programmed and adjusted by your healthcare provider to better match your pain pattern.
Will I feel the stimulation all the time?
Some patients feel a mild tingling sensation, while newer systems may provide pain relief without noticeable sensations.
Can the device be removed if needed?
Yes, spinal cord stimulators can be removed if necessary, especially if the therapy is not effective or complications occur.
Medical References
- Mayo Clinic – Spinal Cord Stimulation
- Cleveland Clinic – Spinal Cord Stimulator Overview
- National Institutes of Health (NIH) – Chronic Pain Management
- American Society of Interventional Pain Physicians (ASIPP) Guidelines
- Johns Hopkins Medicine – Neuromodulation Therapies
Disclaimer
This content is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.